Most people think insulin resistance is a diabetes problem.
It is not.
It is a slow, decades-long shift that starts silently, produces symptoms that nobody connects to blood sugar, and only shows up on a standard lab report after years of compensatory work by the pancreas have finally run out.
By the time fasting glucose flags on a routine panel, insulin resistance has typically been developing for 10 to 15 years.
That’s not a typo. A decade or more of physiological dysfunction — fatigue, cravings, weight resistance, brain fog — before anything shows up on the test your doctor ordered.
Here’s what’s actually happening, why standard testing misses it for so long, and what to look for instead.
What Insulin Resistance Actually Is
Insulin is the hormone your pancreas releases after you eat. Its job is to signal your cells to absorb glucose from the bloodstream and use it for energy. When that signaling works correctly, blood sugar rises after a meal, insulin is released, cells absorb the glucose, and blood sugar returns to baseline.
Insulin resistance is what happens when cells stop responding to that signal efficiently.
The pancreas doesn’t give up immediately. Instead, it compensates — releasing more and more insulin to get the same result. For years, sometimes decades, this compensation keeps blood sugar looking normal on a standard panel. Fasting glucose stays in range. HbA1c stays below the threshold. Your doctor says everything looks fine.
But underneath that normal-looking lab result, insulin levels are running chronically elevated, cells are becoming progressively less responsive, and the metabolic environment is quietly shifting in ways that will eventually become impossible to ignore.
The compensation eventually fails. That’s when fasting glucose finally rises. That’s when the diabetes conversation begins.
But by that point, you’ve been living with insulin resistance for a very long time.
Why Standard Testing Misses It for So Long
The standard blood sugar panel includes two markers: fasting glucose and HbA1c.
Fasting glucose tells you where blood sugar sits after an overnight fast — your metabolic system at rest, with no food influence. It’s a single snapshot taken under the most favorable conditions possible.
HbA1c gives you a 90-day average. Averages are useful but they can look completely normal while hiding significant variability underneath. Someone who spikes to 165 after every meal and crashes to 68 two hours later can average out to a perfectly normal HbA1c.
Neither test measures insulin. Neither test shows you what blood sugar does after a meal. Neither test captures the variability, the spikes, the crashes, or the compensatory hyperinsulinemia that characterizes the early stages of insulin resistance.
The critical missing piece is fasting insulin. When insulin resistance is developing, the pancreas compensates by producing more insulin — so fasting insulin rises years before fasting glucose moves at all. Running fasting insulin alongside fasting glucose and calculating HOMA-IR (a simple ratio of the two numbers) catches insulin resistance at a stage when intervention is most effective and most reversible.
Most standard panels never order fasting insulin. Most people never know.

The 6 Silent Symptoms That Show Up First
This is the part that matters most for most people reading this. Because insulin resistance doesn’t wait silently while the labs look normal. It produces symptoms — specific, recognizable, patterned symptoms — that almost nobody connects to blood sugar.
Post-meal fatigue. A significant energy drop 1 to 2 hours after eating is one of the earliest and most consistent signs of insulin resistance. Cells are struggling to use glucose efficiently, so even though you just ate, you feel depleted rather than fueled. The larger the meal and the more carbohydrate-heavy it was, the more pronounced the crash.
Carbohydrate and sugar cravings. Afternoon and evening cravings for carbohydrates are driven by compensatory insulin swings throughout the day. When blood sugar spikes and then overcorrects downward, the body reads the crash as an emergency and generates an urgent craving for fast glucose. This cycle repeats predictably — often 4 to 5 times daily — and gets stronger as insulin resistance progresses.
Weight that won’t move. High circulating insulin keeps fat locked in storage. Insulin is a fat storage hormone — when it runs chronically elevated, the metabolic environment actively resists fat release regardless of caloric restriction. This is why so many people with unrecognized insulin resistance cannot lose weight despite eating carefully and exercising consistently. The physiology is working against them.
Brain fog. The brain is the most glucose-dependent organ in the body, using approximately 20% of total glucose supply. When glucose delivery becomes inconsistent — spiking after meals and then dropping sharply — cognitive function follows. The inability to concentrate, difficulty finding words, the feeling of thinking through cotton that descends in the mid-morning or mid-afternoon: these are often blood sugar events, not attention problems.
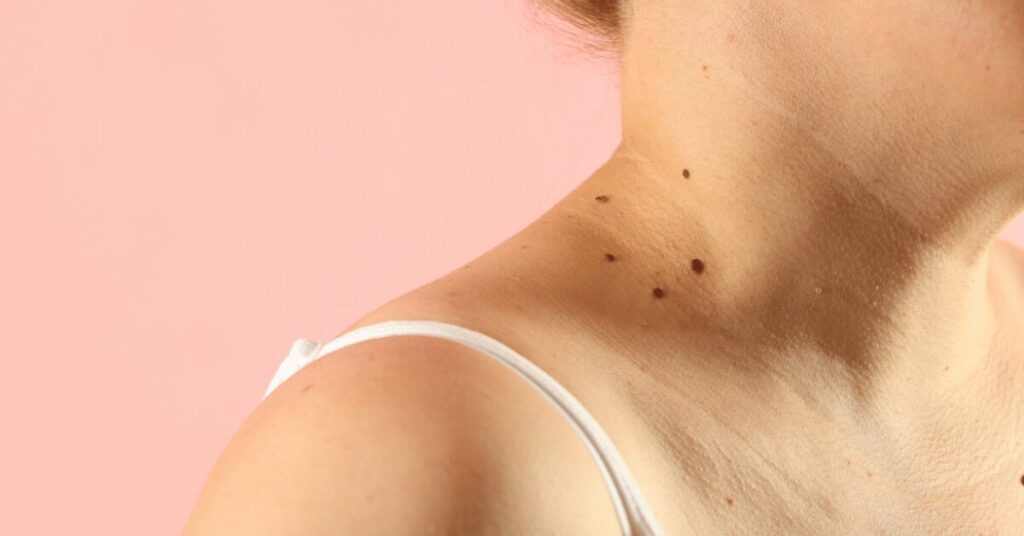
Skin tags and dark patches. This one surprises people. Skin tags — small soft growths that typically appear around the neck, armpits, and groin — and acanthosis nigricans, a darkening and thickening of the skin in skin folds, are both physical signs of hyperinsulinemia. They occur because chronically elevated insulin stimulates cell proliferation and increases melanin production. They’re often dismissed as cosmetic concerns. They’re actually metabolic signals.
Hormonal disruption. Insulin drives ovarian androgen production. In the context of chronic hyperinsulinemia, this manifests as PMS, irregular cycles, hair thinning, and acne — particularly the jaw and chin pattern associated with androgen excess. Many people treat these symptoms hormonally for years without ever investigating the insulin picture driving them.
All of these symptoms can occur with completely normal fasting glucose.
That’s the point.
The Four Stages — and Why Stage 1 and 2 Are Almost Never Caught
Insulin resistance doesn’t arrive suddenly. It progresses through stages, and the earliest stages are almost entirely invisible to standard testing.
Stage 1 is when insulin spikes after meals but fasting values remain completely normal. Excess metabolic fuel begins driving fat storage — including intramuscular fat and early fatty liver — and oxidative stress begins. Standard labs: entirely normal. This stage is the highest reversibility window and almost no one is caught here.
Stage 2 is when fasting insulin becomes elevated — the first lab marker that catches what’s happening. Blood sugar crashes and cravings begin as the system becomes less stable. This is the stage where targeted intervention produces the most significant results. Most practitioners don’t run fasting insulin, so this stage is still largely missed.
Stage 3 is when fasting glucose begins rising and HbA1c climbs above 5.4%. This is where conventional medicine starts paying attention — but the problem has been developing for years at this point.
Stage 4 is metabolic syndrome territory — visceral adiposity, elevated triglycerides, hypertension, progressive beta cell dysfunction. This is the stage where conventional pharmaceutical intervention typically begins.
The functional medicine approach is to catch this at Stage 1 or 2 — when it’s most reversible and least disruptive to address.
If you recognized yourself in more than one of the symptoms above, your cravings and energy patterns may be telling you something specific. The Cravings Root Cause Quiz identifies whether your pattern is metabolic, hormonal, or stress-driven — and explains the physiology behind what your body has been trying to communicate.